Measles is a highly contagious viral infection caused by the Measles virus (Rubeola). While often considered a childhood disease, measles can affect people of all ages, and its severity varies significantly between children and adults. Although vaccination programs have reduced cases worldwide, recent measles outbreaks highlight the importance of understanding its risks, complications, and prevention methods.
Children typically experience mild to moderate symptoms, but measles in adults can lead to more severe complications, including pneumonia and encephalitis. The MMR vaccine (Measles, Mumps, and Rubella) is the most effective way to prevent measles, yet many unvaccinated individuals remain vulnerable to infection.
In this article, we’ll explore the key differences in measles symptoms, risks, and complications between adults and children. We’ll also discuss how measles spreads, the dangers of outbreaks, and essential prevention strategies to protect yourself and your loved ones.
Measles in Adults vs. Children: Key Differences

Symptoms of Measles in Children vs. Adults
Measles symptoms generally follow a similar pattern in both children and adults, but the severity and potential complications can vary significantly between the two groups. Understanding these differences is crucial for early detection, proper treatment, and prevention of severe outcomes.
1. Early Symptoms (Prodromal Phase)
The first signs of measles appear 7-14 days after exposure to the virus. Both children and adults typically experience:
- High fever (often above 101°F or 38.3°C).
- Cough, runny nose, and red, watery eyes (also known as the three C’s—cough, coryza, and conjunctivitis).
- Fatigue and body aches, similar to flu-like symptoms.
However, adults may experience these symptoms more intensely and for a longer duration compared to children.
2. Koplik’s Spots: A Unique Early Sign
A distinguishing feature of measles is the presence of Koplik’s spots—tiny white spots with a bluish-white center inside the mouth, particularly on the inner cheeks. These spots appear 1-2 days before the measles rash and are a key diagnostic sign of the disease.
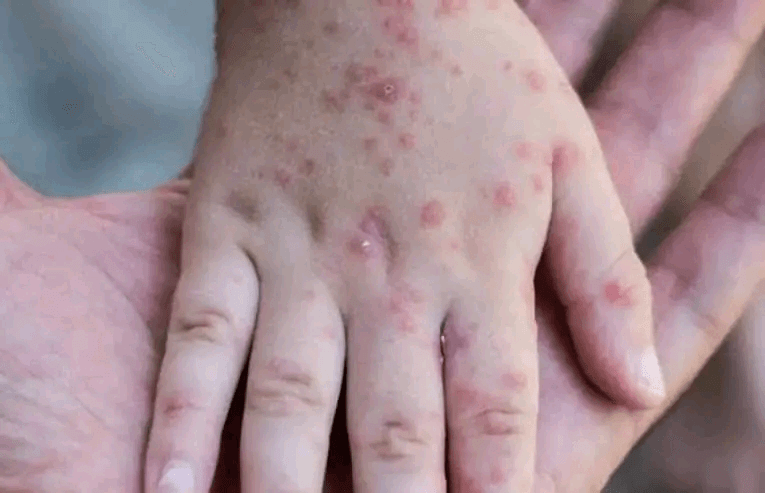
3. Measles Rash: Onset and Progression
The characteristic red, blotchy rash typically begins 3-5 days after initial symptoms and spreads in the following pattern:
- Starts on the face and behind the ears.
- Spreads downward to the neck, torso, arms, and legs.
- Merges into larger patches, making the skin appear inflamed.
- Lasts about a week before fading, often leaving behind temporary brown discoloration and peeling skin.
Children usually recover faster from the rash, while adults may experience more intense skin irritation, swelling, and discomfort.
4. Fever Patterns and Duration
- In children, fever often peaks at the start of the rash and gradually declines.
- In adults, fever tends to stay higher for longer, increasing the risk of dehydration and secondary infections.
5. Severity and Risk of Complications
While measles is often mild in healthy children, adults are at a greater risk of complications, including:
- Severe dehydration and prolonged fatigue.
- Higher likelihood of pneumonia, encephalitis, and hospitalization.
- Longer recovery time and increased risk of post-viral complications.
In contrast, young children—especially those under five—are vulnerable to ear infections, diarrhea, and malnutrition caused by measles.
Key Takeaway
While measles symptoms are generally similar in children and adults, adults tend to experience more severe and prolonged illness, leading to a higher risk of complications. Early recognition and vaccination with the MMR vaccine remain the best defense against this potentially serious disease
How Measles Spreads: Transmission & Risk Factors
Measles is one of the most highly contagious viral infections, capable of spreading rapidly in unvaccinated populations. The virus is primarily transmitted through airborne droplets and direct contact, making it easy to contract in crowded environments. Understanding how measles spreads and the risk factors that increase susceptibility is essential for prevention.
1. How Measles Spreads (Modes of Transmission)
a) Airborne Transmission: The Primary Route
- Measles spreads through tiny respiratory droplets released when an infected person coughs, sneezes, or talks.
- The virus can remain suspended in the air for up to two hours after the infected person has left a room.
- Simply breathing in these virus-laden droplets can cause infection.
b) Direct Contact with Contaminated Surfaces
- Measles can also spread when someone touches contaminated surfaces (such as doorknobs, toys, or utensils) and then touches their face, mouth, or eyes.
- The Measles virus (Rubeola) can survive on surfaces for up to two hours.
c) Highly Contagious Nature of Measles
- Measles has an extremely high transmission rate—around 90% of unvaccinated individuals who are exposed to the virus will become infected.
- Infected individuals are contagious 4 days before the rash appears and up to 4 days after.
- The virus can easily spread in schools, daycare centers, hospitals, and public places if proper precautions are not taken.
2. Who Is at Risk? Key Risk Factors for Measles Infection
a) Unvaccinated Individuals
- The MMR vaccine (Measles, Mumps, and Rubella) provides lifelong immunity in most cases.
- People who have not received two doses of the MMR vaccine are at the highest risk of contracting measles.
- Infants under 12 months (who are too young for vaccination) are especially vulnerable.
b) People with Weakened Immune Systems
- Individuals with HIV/AIDS, cancer, or autoimmune diseases are more susceptible to severe measles infections.
- Those undergoing chemotherapy, organ transplants, or immunosuppressive therapy have a higher risk of complications.
c) Travel to Measles-Endemic Regions
- Measles remains endemic in certain countries with low vaccination rates.
- Travelers to regions experiencing measles outbreaks are at increased risk and should ensure vaccination before traveling.
d) Close Contact with an Infected Person
- Living in crowded environments (such as dormitories, refugee camps, or military barracks) increases exposure risk.
- Healthcare workers, caregivers, and family members of infected individuals are more likely to contract the virus.
Key Takeaway
Measles spreads through the air and direct contact, making it highly contagious among unvaccinated and immunocompromised individuals. The best way to prevent measles transmission is through vaccination, good hygiene, and avoiding contact with infected individuals. Understanding how measles spreads and recognizing risk factors can help reduce outbreaks and protect vulnerable populations.
Measles Recovery Time and Long-Term Effects
Recovering from measles varies from person to person, depending on factors such as age, overall health, and immune system strength. While most healthy individuals recover within a few weeks, measles can leave lasting effects, especially in adults, young children, and immunocompromised individuals. Understanding the recovery process and potential long-term complications can help in managing symptoms and preventing serious health risks.
1. Measles Recovery Time: What to Expect
a) Timeline of Measles Recovery
Measles typically follows a two-stage progression, with symptoms developing over 2-3 weeks:
- Incubation Period (7-14 Days)
- After exposure, the virus remains in the body without visible symptoms.
- During this time, the infected person is not yet contagious.
- Prodromal Stage (Days 1-4 of Symptoms)
- Fever, cough, runny nose, and red eyes appear.
- Koplik’s spots (small white spots inside the mouth) may be noticeable.
- Rash Stage (Days 4-10 of Symptoms)
- A red, blotchy rash appears, starting on the face and spreading downward.
- Fever peaks and then gradually declines as the rash begins to fade.
- The rash lasts about 6-7 days before drying out and peeling.
- Recovery Phase (Up to 3 Weeks After Rash Fades)
- Fatigue and lingering cough may persist for several weeks.
- Skin discoloration where the rash was present can take time to fade.
- The immune system remains weakened, increasing susceptibility to secondary infections.
b) Recovery Differences in Children vs. Adults
- Children with healthy immune systems usually recover faster, but young children under 5 may be at risk for complications.
- Adults often experience a longer recovery period, with more intense symptoms and a higher likelihood of developing severe complications.
2. Long-Term Effects of Measles: Potential Health Risks
While most individuals recover fully, measles can lead to serious long-term complications, especially in those with weakened immune systems.
a) Secondary Infections and Organ Damage
Measles weakens the immune system, leaving individuals vulnerable to:
- Bacterial pneumonia – a leading cause of measles-related deaths.
- Ear infections – can result in permanent hearing loss.
- Severe diarrhea and dehydration, especially in children.
b) Neurological Complications: Brain Infections
- Acute Encephalitis (1 in 1,000 cases)
- A dangerous brain inflammation that can cause seizures, brain damage, or death.
- Subacute Sclerosing Panencephalitis (SSPE) (1 in 10,000-100,000 cases)
- A rare but fatal neurological disorder that develops years after measles infection.
- Leads to memory loss, personality changes, seizures, and brain deterioration.
c) Immune System Suppression: Increased Disease Risk
- Measles causes immune amnesia, which weakens immunity against other infections for months or even years.
- Studies suggest that measles erases immunity to previous infections, making survivors more prone to tuberculosis, pneumonia, and other diseases.
d) Pregnancy Complications
- Pregnant women with measles are at a higher risk of miscarriage, preterm labor, and low birth weight babies.
- Measles infection during pregnancy can also lead to congenital measles in newborns.
3. How to Support Recovery and Prevent Complications
- Stay Hydrated & Rest – Fluids help prevent dehydration, and rest allows the immune system to recover.
- Vitamin A Supplements – The WHO recommends Vitamin A for children with measles to reduce complications.
- Monitor for Warning Signs – Seek medical attention for persistent fever, difficulty breathing, seizures, or confusion.
- Strengthen Immunity – A healthy diet, proper hygiene, and vaccination help prevent reinfection and complications.
Key Takeaway
While most people recover from measles within 2-3 weeks, the virus can weaken the immune system, leaving individuals at risk for severe infections, neurological damage, and long-term health issues. The best way to prevent complications and outbreaks is through vaccination and early treatment.
Risks and Complications of Measles
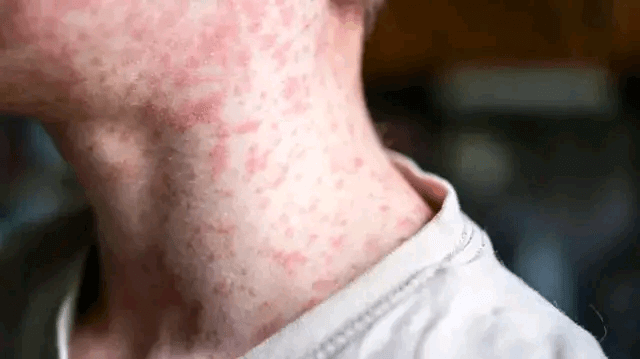
Common Complications in Children
While measles is often thought of as a mild childhood disease, it can lead to serious complications, especially in children under five years old or those with weakened immune systems. In some cases, these complications can result in hospitalization, long-term health issues, or even death. Understanding the most common measles-related complications in children can help parents and caregivers recognize warning signs and seek medical attention early.
1. Respiratory Complications: Pneumonia and Ear Infections
a) Pneumonia: The Leading Cause of Measles-Related Death in Children
- Measles suppresses the immune system, making children vulnerable to bacterial and viral pneumonia.
- Pneumonia occurs in about 1 in 20 children with measles.
- Symptoms include persistent cough, chest pain, difficulty breathing, and high fever.
- Severe pneumonia can be life-threatening, especially in malnourished or immunocompromised children.
b) Ear Infections and Hearing Loss
- Around 1 in 10 children with measles develop a middle ear infection (otitis media).
- Caused by bacterial growth due to fluid buildup in the ears.
- Can lead to temporary or permanent hearing loss if left untreated.
2. Digestive Complications: Severe Diarrhea and Malnutrition
a) Diarrhea and Dehydration
- 8% of children with measles experience severe diarrhea, leading to rapid dehydration.
- Dehydration can cause fatigue, dry mouth, sunken eyes, and reduced urination.
- Infants and toddlers are at the highest risk due to their smaller fluid reserves.
b) Malnutrition and Vitamin A Deficiency
- Measles can reduce appetite and cause digestive issues, leading to weight loss and malnutrition.
- Vitamin A deficiency is common in children with measles and increases the risk of blindness and severe infection.
- The WHO recommends Vitamin A supplements for all children with measles to prevent severe complications.
3. Neurological Complications: Encephalitis and Brain Damage
a) Measles-Induced Encephalitis (1 in 1,000 Cases)
- A rare but severe brain inflammation that can occur during or after measles infection.
- Symptoms include seizures, confusion, high fever, and loss of consciousness.
- Can lead to permanent brain damage, developmental delays, or epilepsy.
b) Subacute Sclerosing Panencephalitis (SSPE) (1 in 10,000–100,000 Cases)
- A fatal, progressive brain disorder that appears years after measles infection.
- Leads to memory loss, behavioral changes, seizures, and loss of motor skills.
- More common in children who had measles before the age of two.
4. Weakened Immune System: Increased Risk of Other Infections
- Measles weakens the immune system for weeks to months after infection.
- Children who recover from measles have a higher risk of catching other infections like tuberculosis, pneumonia, and skin infections.
- This is known as “immune amnesia,” where measles erases the body’s memory of past immunity to diseases.
5. Measles Complications in Malnourished and Unvaccinated Children
- Malnourished children, especially those in developing countries, are at higher risk of severe measles complications.
- In regions with poor healthcare, measles mortality rates can reach up to 10%.
- Herd immunity from vaccination protects unvaccinated children by reducing overall disease spread.
Key Takeaway
While most children recover from measles, serious complications like pneumonia, encephalitis, and malnutrition can occur, especially in young, unvaccinated, or immunocompromised children. Early medical intervention, hydration, and proper nutrition can help reduce risks, but the best prevention method remains the MMR vaccine, which provides lifelong immunity and protection against measles-related complications.
Severe Complications in Adults
While measles is commonly associated with childhood infections, adults are at a higher risk of experiencing severe complications. The immune response to the Measles virus (Rubeola) tends to be more intense in adults, leading to a higher likelihood of hospitalization, long-term health issues, and even fatal outcomes. Individuals who are unvaccinated, immunocompromised, or pregnant are particularly vulnerable to serious complications.
1. Respiratory Complications: Pneumonia and Severe Breathing Issues
a) Measles-Related Pneumonia (Most Common Cause of Death in Adults)
- Pneumonia is the leading cause of measles-related death in adults.
- 1 in 20 measles cases in adults results in pneumonia, making it one of the most severe complications.
- Measles suppresses the immune system, allowing bacterial or viral pneumonia to develop.
- Symptoms include chest pain, difficulty breathing, high fever, and persistent cough.
b) Acute Respiratory Distress Syndrome (ARDS)
- A rare but life-threatening lung condition caused by severe inflammation.
- Leads to fluid buildup in the lungs, preventing oxygen from reaching the bloodstream.
- Often requires intensive care and mechanical ventilation for survival.
2. Neurological Complications: Encephalitis and Brain Damage
a) Measles Encephalitis (1 in 1,000 Cases in Adults)
- A severe inflammation of the brain that can develop during or after a measles infection.
- Symptoms include seizures, confusion, difficulty walking, and unconsciousness.
- Can lead to permanent brain damage, memory loss, or cognitive impairment.
b) Subacute Sclerosing Panencephalitis (SSPE) (1 in 10,000–100,000 Cases)
- A delayed, fatal brain disorder that appears years after measles infection.
- Causes progressive memory loss, muscle spasms, behavioral changes, and paralysis.
- Once symptoms begin, SSPE is always fatal, usually within 1-3 years.
3. Cardiovascular Complications: Increased Risk of Heart Issues
a) Myocarditis (Heart Inflammation)
- Measles can cause inflammation of the heart muscle (myocardium), leading to irregular heartbeats and heart failure.
- Symptoms include chest pain, shortness of breath, and extreme fatigue.
b) Increased Stroke and Heart Attack Risk
- Studies suggest that measles-induced immune suppression can trigger blood vessel inflammation, increasing the risk of stroke or heart attack.
4. Immune System Suppression: High Risk of Secondary Infections
- Measles weakens the immune system, making adults prone to bacterial infections like:
- Severe bacterial pneumonia
- Tuberculosis reactivation
- Skin infections and sepsis (blood poisoning)
- This immune suppression can last for months to years, leaving adults vulnerable to other diseases.
5. Measles Complications in Pregnant Women
a) High Risk of Pregnancy-Related Complications
- Pregnant women with measles face higher risks of miscarriage, preterm birth, and stillbirth.
- The virus can cross the placenta, leading to congenital measles in newborns.
- Measles infection during pregnancy can also cause low birth weight and developmental problems.
b) Congenital Measles in Newborns
- If a mother contracts measles during pregnancy, the baby may be born with congenital measles, leading to:
- Severe pneumonia
- Brain inflammation
- Lifelong immune system weakness
6. Vision and Hearing Loss
a) Blindness Due to Measles
- Measles can cause corneal ulcers and severe eye infections, leading to permanent vision loss.
- This is more common in adults with Vitamin A deficiency or pre-existing eye conditions.
b) Permanent Hearing Loss
- Measles-related ear infections or nerve damage can cause irreversible hearing loss in adults.
- Some cases result from measles encephalitis, which affects the auditory nerves.
7. Longer Recovery and Increased Mortality in Adults
- Adults take longer to recover from measles compared to children.
- Severe fatigue, persistent cough, and weakened immunity can last for weeks to months after recovery.
- Mortality rates in adults are higher, especially in individuals with chronic diseases or weak immune systems.
Key Takeaway
While measles is often mild in children, it can lead to life-threatening complications in adults, particularly those who are unvaccinated, immunocompromised, or pregnant. Neurological damage, pneumonia, immune suppression, and heart complications are more severe in adults, making vaccination the most effective prevention method. If an adult contracts measles, early medical care is crucial to reduce the risk of severe complications.
Impact of Measles Outbreaks
Measles outbreaks have far-reaching consequences, affecting public health, healthcare systems, economies, and vulnerable populations. Since measles is one of the most contagious viruses known, outbreaks can spread rapidly in communities with low vaccination rates, leading to severe complications, increased healthcare costs, and social disruptions.
Understanding the impact of measles outbreaks is essential for preventing widespread infections and strengthening immunization efforts.
1. Public Health Consequences
a) Rapid Transmission and High Infection Rates
- Measles spreads extremely fast, with a 90% infection rate among unvaccinated individuals who come into contact with the virus.
- A single infected person can spread the virus to 12–18 others, making it one of the most contagious diseases.
- Outbreaks often start in schools, daycare centers, airports, and crowded public spaces.
b) High Morbidity and Mortality Rates
- While most healthy individuals recover, measles leads to severe complications in young children, older adults, pregnant women, and immunocompromised individuals.
- The World Health Organization (WHO) reports that measles kills over 100,000 people worldwide each year, mainly in areas with low vaccination rates.
- Hospitalization rates during outbreaks increase, straining medical resources.
c) Immune Suppression & Increased Susceptibility to Other Diseases
- Measles damages the immune system for months to years, making survivors vulnerable to infections like pneumonia, tuberculosis, and diarrheal diseases.
- This “immune amnesia” effect means that people who have had measles may lose immunity to diseases they were previously protected against.
2. Strain on Healthcare Systems
a) Overcrowding in Hospitals and Medical Facilities
- During outbreaks, hospitals experience a surge in measles-related admissions, increasing bed shortages and resource allocation issues.
- Doctors and nurses are overwhelmed, delaying care for other medical conditions.
- In severe outbreaks, temporary quarantine zones or isolation wards may be needed to control the spread.
b) Increased Demand for Medical Supplies & Services
- Outbreaks increase demand for vaccines, antiviral medications, IV fluids, oxygen support, and intensive care units (ICUs).
- Countries with weaker healthcare infrastructures struggle to manage large outbreaks, leading to higher mortality rates.
c) Economic Burden on Healthcare Systems
- Treating measles complications such as pneumonia, encephalitis, and hospital stays adds financial pressure to both public and private healthcare systems.
- The CDC estimates that each measles case costs the healthcare system thousands of dollars, especially if hospitalization is required.
3. Economic and Social Disruptions
a) Impact on Work and Productivity
- When measles outbreaks occur, infected individuals and their families miss work, leading to lost wages and productivity.
- Employers face workforce shortages, particularly in essential services like healthcare, education, and transportation.
b) School Closures and Disruptions in Education
- Measles outbreaks often lead to school closures, disrupting education for students and forcing parents to take time off work.
- Unvaccinated children may be excluded from schools and public spaces to prevent the virus from spreading.
c) Travel Restrictions and Quarantines
- During major outbreaks, governments may impose travel bans, quarantines, or public gathering restrictions to contain the virus.
- Airlines and tourism industries suffer losses due to reduced travel demand in affected regions.
- Measles outbreaks in airports, cruise ships, or international events can result in rapid global spread.
4. Vulnerable Populations at Greatest Risk
a) Unvaccinated Communities & Anti-Vaccine Movements
- Outbreaks are more common in communities with low vaccination rates, often influenced by anti-vaccine misinformation.
- Herd immunity requires at least 95% of the population to be vaccinated, but vaccine hesitancy has led to resurgent measles outbreaks in many countries.
b) Developing Countries with Limited Healthcare Access
- In low-income nations, measles remains a leading cause of childhood mortality due to lack of vaccines, poor nutrition, and limited healthcare facilities.
- Countries facing war, displacement, or natural disasters struggle to maintain vaccination programs, making outbreaks harder to control.
c) Immunocompromised Individuals & Pregnant Women
- Measles poses life-threatening risks to cancer patients, organ transplant recipients, HIV/AIDS patients, and pregnant women.
- Pregnant women with measles are at risk of miscarriage, premature birth, and congenital measles in newborns.
5. The Role of Vaccination in Preventing Outbreaks
a) Effectiveness of the Measles Vaccine (MMR Vaccine)
- The Measles, Mumps, and Rubella (MMR) vaccine is 97% effective after two doses.
- Countries with high vaccination rates have almost eliminated measles, but gaps in immunization coverage lead to outbreaks.
b) Importance of Herd Immunity
- When 95% or more of the population is vaccinated, measles outbreaks become extremely rare.
- Unvaccinated individuals, including infants and those with medical conditions, are protected through herd immunity.
- Vaccine campaigns and public health awareness programs are key to stopping measles outbreaks.
Key Takeaway
Measles outbreaks have serious consequences for public health, economies, and social systems. Rapid transmission, severe complications, healthcare strain, and economic losses highlight the importance of vaccination programs. By ensuring high immunization rates, promoting public awareness, and strengthening global health initiatives, measles outbreaks can be prevented, protecting both individuals and communities from this highly contagious disease.
Prevention and Treatment of Measles

Measles Vaccine: How It Works and Why It’s Essential
The measles vaccine is the most effective way to prevent measles infections, complications, and outbreaks. Since its introduction, the vaccine has dramatically reduced measles cases worldwide and saved millions of lives. However, in recent years, vaccine hesitancy and declining immunization rates have led to resurgences of measles outbreaks, emphasizing the continued need for widespread vaccination.
Understanding how the measles vaccine works, its benefits, and why it is essential can help promote public confidence in immunization efforts and prevent the spread of this highly contagious disease.
1. How the Measles Vaccine Works
The measles vaccine is a live attenuated vaccine, meaning it contains a weakened form of the measles virus that stimulates the immune system without causing the disease.
a) Immune Response to the Vaccine
- When the vaccine is administered, the immune system recognizes the weakened virus and begins producing antibodies against it.
- These antibodies remain in the body, providing long-term immunity against future measles infections.
- If a vaccinated person is exposed to measles later in life, their immune system can quickly recognize and fight off the virus, preventing illness.
b) Vaccine Schedule and Dosage
The Measles, Mumps, and Rubella (MMR) vaccine is the standard immunization used to protect against measles. The recommended schedule includes:
- First dose: Given at 12–15 months of age.
- Second dose: Given at 4–6 years of age.
For those who have not been vaccinated in childhood, two doses in adulthood (at least 28 days apart) can still provide full protection.
- Effectiveness:
- One dose of the MMR vaccine is about 93% effective.
- Two doses provide 97% protection for life.
- Booster Shots:
- In most cases, two doses provide lifelong immunity.
- However, booster shots may be recommended for immunocompromised individuals or during outbreaks.
2. Why the Measles Vaccine Is Essential
a) Preventing Severe Complications and Death
- Measles is not a mild disease—it can lead to serious complications such as pneumonia, encephalitis (brain inflammation), blindness, and death.
- Before vaccines, millions of people contracted measles each year, leading to thousands of deaths.
- According to the World Health Organization (WHO), measles vaccination prevented approximately 56 million deaths between 2000 and 2021.
b) Protecting Vulnerable Populations
- Some individuals cannot receive the measles vaccine due to medical conditions, allergies, or weakened immune systems (e.g., cancer patients, newborns, or people with HIV/AIDS).
- These individuals rely on herd immunity, meaning when enough people are vaccinated, the virus cannot spread easily, protecting those who are most vulnerable.
c) Controlling and Eliminating Measles Worldwide
- Countries with high vaccination rates have successfully eliminated measles as a major health threat.
- However, declining vaccination rates have led to outbreaks in regions where measles was previously eradicated.
- Eradicating measles requires maintaining at least 95% vaccination coverage globally.
d) Economic and Social Benefits
- Treating measles cases is far more expensive than preventing them through vaccination.
- Hospitalization, missed work or school, and outbreak control measures place a huge financial burden on healthcare systems and families.
- Measles vaccines are cost-effective, saving billions of dollars in medical expenses and lost productivity.
3. Addressing Vaccine Hesitancy and Myths
Despite the overwhelming benefits of the measles vaccine, misinformation and vaccine hesitancy have contributed to declining immunization rates in some areas.
a) Myth: “Measles Is a Mild Disease, So Vaccination Isn’t Necessary.”
- Fact: Measles can cause severe complications, hospitalization, and death, especially in young children, older adults, and immunocompromised individuals.
b) Myth: “The MMR Vaccine Causes Autism.”
- Fact: There is no scientific evidence linking the MMR vaccine to autism. The original study that suggested a link has been debunked and retracted, and multiple studies have confirmed that the vaccine is safe.
c) Myth: “Natural Immunity Is Better Than Vaccine Immunity.”
- Fact: While natural infection may provide lifelong immunity, it comes at a high cost—including severe illness, hospitalization, and even death. The vaccine provides strong immunity without the risks of infection.
d) Myth: “The Vaccine Contains Harmful Ingredients.”
- Fact: The MMR vaccine contains only safe, approved ingredients, and does not contain mercury, aluminum, or preservatives that pose health risks.
4. Global Efforts to Increase Measles Vaccination
a) WHO & UNICEF Immunization Campaigns
- Organizations like the WHO, UNICEF, and CDC work globally to provide free or low-cost measles vaccines to underprivileged communities.
- In 2021 alone, over 24 million children missed routine measles vaccines, leading to increased risk of outbreaks.
- Vaccination campaigns focus on boosting immunization rates in developing countries and refugee populations.
b) School and Workplace Vaccination Requirements
- Many countries require proof of measles vaccination for school entry and certain jobs.
- Workplace vaccination programs help increase immunity in healthcare settings, travel industries, and public services.
c) Travel Recommendations & Outbreak Prevention
- Travelers to areas with active measles outbreaks should ensure they are fully vaccinated before departure.
- Outbreak control strategies include rapid vaccination campaigns, isolation of infected individuals, and public awareness programs.
Key Takeaway
The measles vaccine is a safe, effective, and essential tool in preventing measles infections, complications, and outbreaks. With 97% effectiveness after two doses, it not only protects individuals but also helps achieve herd immunity, safeguarding those who cannot be vaccinated.
Increasing global vaccination rates is the only way to eliminate measles and prevent its devastating impact on public health, healthcare systems, and economies. Widespread immunization efforts must continue to combat vaccine misinformation, address hesitancy, and ensure all communities have access to life-saving vaccines.
Managing Symptoms at Home
Measles is a viral infection, meaning there is no specific antiviral treatment to cure the disease. Instead, symptom management is crucial to help the body fight off the infection while preventing complications. Most measles cases resolve within 10–14 days, but proper home care can ease discomfort, speed up recovery, and reduce the risk of complications.
If you or a loved one has measles, follow these home remedies and supportive care tips to manage symptoms effectively.
1. Rest and Hydration
a) Get Plenty of Rest
- Measles weakens the immune system, making the body more susceptible to other infections.
- Adequate sleep allows the body to focus on fighting the virus.
- Reduce physical activity to avoid fatigue and energy depletion.
b) Stay Hydrated
- Fever and sweating can lead to dehydration, making symptoms worse.
- Drink plenty of water, herbal teas, diluted fruit juices, or broths to maintain hydration.
- Watch for signs of dehydration, such as dry mouth, dark urine, and dizziness.
c) Use Electrolyte Solutions
- If vomiting or diarrhea occurs, use oral rehydration solutions (ORS) to replenish lost fluids and electrolytes.
- Coconut water and sports drinks can also help restore hydration levels.
2. Relieving Fever and Body Aches
a) Use Fever-Reducing Medications
- Acetaminophen (Tylenol) or ibuprofen (Advil, Motrin) can help reduce fever, headaches, and muscle pain.
- Avoid aspirin in children, as it can cause Reye’s syndrome, a rare but serious condition.
b) Keep the Body Cool
- Wear light, breathable clothing to prevent overheating.
- Use a lukewarm sponge bath or a damp washcloth on the forehead to lower body temperature.
- Avoid cold showers or ice baths, as they can cause shivering and worsen discomfort.
c) Use Natural Remedies for Pain Relief
- Herbal teas with chamomile or ginger may help soothe body aches and headaches.
- A warm compress can relieve muscle tension and joint pain.
3. Easing Cough and Sore Throat
a) Stay in a Humid Environment
- Dry air can worsen cough and throat irritation.
- Use a humidifier or place a bowl of hot water in the room to add moisture to the air.
- Taking a warm shower can also help loosen mucus and relieve throat discomfort.
b) Drink Warm Fluids
- Warm herbal teas, honey and lemon water, or warm broth can soothe the throat and reduce irritation.
- Avoid caffeinated or sugary drinks, as they can cause dehydration and increase throat dryness.
c) Use Natural Cough Remedies
- Honey (for children over one year and adults) is an effective natural remedy for soothing coughs.
- Saltwater gargles (1/2 teaspoon of salt in a glass of warm water) can reduce throat inflammation and discomfort.
- Menthol or eucalyptus lozenges can provide temporary relief from a sore throat.
4. Protecting the Eyes from Sensitivity
a) Dim the Lights
- Measles causes light sensitivity (photophobia), making bright lights uncomfortable.
- Keep the room dimly lit and use soft lighting instead of harsh bulbs.
b) Wear Sunglasses Indoors
- If the eyes are extremely sensitive, wearing dark sunglasses indoors can help reduce discomfort.
c) Use Warm Compresses for Eye Discomfort
- Soak a clean cloth in warm water, wring it out, and place it gently over the eyes for relief.
d) Avoid Rubbing the Eyes
- Measles can cause conjunctivitis (pink eye), leading to itching and irritation.
- To prevent further irritation or infection, avoid touching or rubbing the eyes.
5. Strengthening the Immune System
a) Eat Nutritious Foods
- While appetite may be reduced, eating nutrient-dense foods helps support the immune system.
- Focus on:
- Fruits and vegetables rich in vitamin C (oranges, strawberries, bell peppers).
- Protein-rich foods (chicken soup, eggs, lentils) for healing.
- Foods high in zinc (nuts, seeds, whole grains) to support immunity.
b) Take Vitamin A Supplements (If Recommended by a Doctor)
- Vitamin A deficiency increases the risk of severe measles complications.
- The World Health Organization (WHO) recommends high-dose vitamin A supplements for children with measles, especially in developing countries.
6. Preventing the Spread of Measles at Home
Since measles is highly contagious, it’s essential to prevent the virus from spreading to others in the household.
a) Isolate the Sick Person
- Keep the infected person in a separate room for at least 4 days after the rash appears to reduce transmission.
- Limit contact with young children, elderly individuals, and immunocompromised family members.
b) Practice Good Hygiene
- Wash hands frequently with soap and water for at least 20 seconds.
- Disinfect commonly touched surfaces like doorknobs, light switches, and countertops.
- Cover coughs and sneezes with a tissue or elbow to prevent airborne spread.
c) Avoid Visitors
- Family and friends should wait until full recovery before visiting to prevent infection.
- If necessary, virtual communication (video calls, messages) can help the sick person stay connected.
7. When to Seek Medical Attention
While most measles cases can be managed at home, seek medical help immediately if any of the following occur:
- Difficulty breathing or persistent cough (signs of pneumonia).
- Severe dehydration (no urination, extreme weakness, confusion).
- Seizures or loss of consciousness (potential encephalitis).
- High fever lasting more than 5 days or returning after initial improvement.
- Persistent vomiting or inability to keep fluids down.
Key Takeaway
Managing measles symptoms at home involves rest, hydration, fever management, and immune support. Since measles has no cure, symptom relief and supportive care are essential for a smoother recovery. Preventing complications and avoiding the spread of infection can protect both the sick individual and those around them. However, if symptoms become severe, immediate medical attention is crucial to prevent life-threatening complications.
When to Seek Medical Help
While most cases of measles can be managed at home with appropriate care, there are instances where medical intervention is necessary to prevent complications or treat serious symptoms. Since measles can lead to severe complications like pneumonia, encephalitis (brain inflammation), and dehydration, it is crucial to recognize warning signs early and seek medical care when needed.
Understanding when to seek professional medical attention can help prevent the disease from progressing into life-threatening situations.
1. Difficulty Breathing or Severe Cough
a) Signs of Respiratory Distress
- Measles can lead to pneumonia, a potentially fatal complication that affects the lungs and makes it difficult to breathe.
- Difficulty breathing can be a sign that the virus has spread to the lungs or that a secondary infection, like pneumonia or bronchitis, has developed.
- Wheezing, shortness of breath, or rapid breathing should be addressed immediately.
- Severe cough that worsens over time, or if it is accompanied by chest pain or a feeling of tightness, may require medical attention.
b) Emergency Signs
- If the person is struggling to breathe, showing signs of blue lips or face, or unable to take in air, call emergency services immediately. These could be signs of respiratory failure or severe pneumonia that require urgent care.
2. Dehydration or Difficulty Keeping Fluids Down
a) Signs of Dehydration
- Dehydration is a serious concern during measles due to fever, vomiting, and diarrhea, which can lead to rapid fluid loss.
- Look for signs of dehydration, including:
- Dry mouth and throat
- Reduced urination or dark-colored urine
- Extreme thirst
- Dizziness or confusion
- Tiredness or lethargy
b) When to Seek Medical Help
- If the person is unable to drink fluids or keep fluids down due to vomiting or nausea, seek medical attention immediately.
- In severe cases, dehydration can lead to kidney failure, shock, or unconsciousness, all of which require urgent medical care.
3. Persistent or High Fever
a) Uncontrolled Fever
- A high fever (above 104°F / 40°C) that does not respond to fever-reducing medications (like acetaminophen or ibuprofen) may indicate a secondary bacterial infection or other complications.
- A fever lasting for more than 5 days or one that reappears after initially subsiding can be a red flag that needs medical evaluation.
b) Seizures from High Fever
- In some cases, a very high fever can cause febrile seizures, which are most common in children under the age of 5.
- Signs of a febrile seizure include shaking or twitching, rolling eyes, and unconsciousness.
- If you observe any seizure activity, seek medical help immediately to prevent complications and ensure proper care.
4. Neurological Symptoms or Changes in Mental Status
a) Signs of Encephalitis (Brain Inflammation)
- Encephalitis is a rare but severe complication of measles that can lead to permanent brain damage or death.
- Symptoms include:
- Severe headache
- Confusion or disorientation
- Sensitivity to light (photophobia)
- Stiff neck or difficulty moving
- Severe drowsiness or inability to wake up
- Seizures
b) Behavioral or Cognitive Changes
- If a person with measles begins to experience confusion, becomes unresponsive, or displays abnormal behavior, this could be a sign of encephalitis or another serious complication.
- Immediate medical attention is essential to treat these conditions and minimize long-term effects.
5. Persistent Eye Problems or Vision Loss
a) Eye Complications from Measles
- Measles can cause eye infections, such as conjunctivitis (pink eye) and keratitis (inflammation of the cornea).
- These infections can lead to vision problems or even permanent blindness if not treated promptly.
- Painful, swollen eyes, blurred vision, or severe light sensitivity should be examined by a healthcare provider.
b) Vision Loss or Severe Eye Discomfort
- If the individual experiences sudden vision changes, difficulty seeing, or loss of vision, seek immediate medical attention. This could indicate a serious eye complication or infection that requires urgent treatment.
6. Skin Rash or Secondary Infections
a) Severe or Uncontrolled Rash
- While a rash is a characteristic symptom of measles, severe rashes that spread rapidly or become infected can require medical intervention.
- If the rash turns into open sores or becomes very painful, there may be a risk of bacterial infections, such as cellulitis.
b) Signs of Secondary Bacterial Infections
- A rash accompanied by pus-filled blisters, swelling, or red streaks could indicate an underlying bacterial infection that requires antibiotics.
- Consult a doctor immediately if any of these signs develop.
7. Worsening or New Symptoms During Recovery
a) Relapse of Symptoms
- Measles typically follows a predictable course, but some individuals experience a relapse of symptoms after an apparent recovery.
- Return of fever, cough, or rash after improvement could indicate that the infection is progressing or that a secondary infection has developed.
b) Unexplained Pain or Discomfort
- If new symptoms such as unexplained pain, swelling, or worsening fatigue emerge, these could signal complications like pneumonia, ear infections, or liver issues.
- Seek medical care to assess these changes and prevent further issues.
8. Special Considerations for Pregnant Women
- Measles can be especially dangerous for pregnant women, leading to miscarriage, premature birth, or low birth weight.
- If a pregnant woman contracts measles, immediate medical intervention is necessary to protect both her and the baby.
- Pregnant women should also be monitored for signs of dehydration, severe fever, or complications.
Key Takeaway
Measles may appear to be a straightforward viral infection in some cases, but its potential to lead to severe complications makes it crucial to recognize when medical intervention is needed. If you or someone you are caring for experiences difficulty breathing, severe dehydration, high fever, neurological symptoms, or persistent pain, it is important to seek medical care immediately. Early intervention can prevent the disease from progressing to more serious health issues and ensure a quicker recovery.
conclusion
Measles is a serious contagious disease that can affect both children and adults, though the risks and complications often vary by age. For children, measles can lead to severe complications such as pneumonia, ear infections, and encephalitis, especially if they are under-vaccinated or have weakened immune systems. While adults typically experience a more intense form of the disease, they are also at risk for life-threatening complications like pneumonia, liver damage, and encephalitis. The impact of measles on adults can be more severe, leading to longer recovery times and increased health risks.
Fortunately, measles is preventable through vaccination, which remains the most effective strategy to protect both children and adults from this potentially deadly virus. The MMR vaccine provides long-lasting immunity and plays a vital role in reducing the spread of the disease. By ensuring that individuals of all ages are vaccinated and practicing proper hygiene and isolation during outbreaks, we can significantly reduce the incidence of measles worldwide.
While measles remains a serious threat, the key to combating this disease lies in prevention, early diagnosis, and prompt medical care. Recognizing symptoms early and seeking timely medical attention can help mitigate the risks associated with the disease, especially for vulnerable populations. By remaining vigilant, promoting vaccination, and adhering to recommended health guidelines, we can continue to protect our communities from the spread of measles and its complications.
Ultimately, prevention is better than cure, and with the widespread availability of the measles vaccine, we have the tools to eradicate this preventable disease and keep future generations safe.