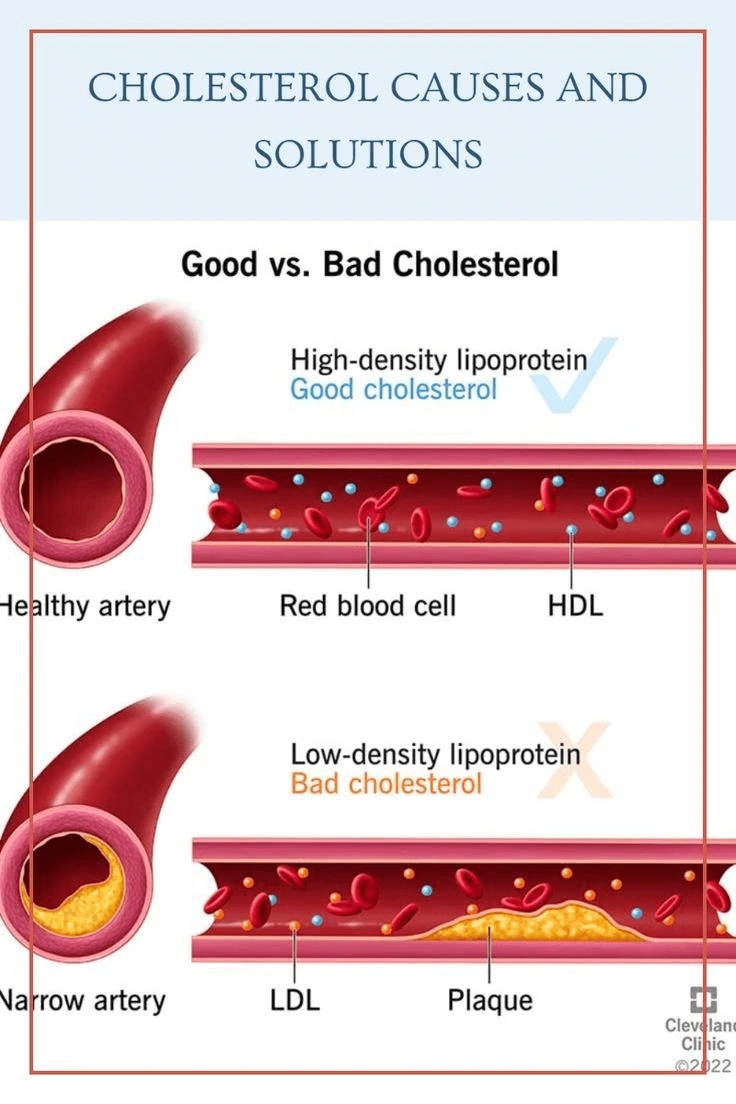
Cholesterol is a crucial component of your body, playing a vital role in building cells, producing hormones, and aiding digestion. However, maintaining balanced cholesterol levels is essential for heart health. Too much low-density lipoprotein (LDL), often called “bad cholesterol,” can lead to plaque buildup in arteries, increasing the risk of heart disease and stroke. On the other hand, high-density lipoprotein (HDL), known as “good cholesterol,” helps remove excess cholesterol from the bloodstream.
Understanding what’s considered normal cholesterol levels, the risks of high cholesterol, and how to manage it effectively is key to maintaining overall well-being. In this article, we’ll break down what’s normal, what’s not, and the best ways to improve your cholesterol levels naturally and medically. Whether you’re looking to make lifestyle changes or explore medical options, this guide will provide the insights you need for better heart health.
Understanding Cholesterol Levels
What Is Cholesterol? (Definition and Role in the Body)
Cholesterol is a fat-like, waxy substance found in every cell of the body. It is essential for several biological functions, including:
- Cell Structure and Function: Cholesterol is a key component of cell membranes, providing stability and flexibility to cells.
- Hormone Production: It plays a crucial role in the production of hormones such as estrogen, testosterone, and cortisol, which regulate various body functions.
- Vitamin D Synthesis: Cholesterol is necessary for the body to produce vitamin D when the skin is exposed to sunlight.
- Bile Production for Digestion: The liver uses cholesterol to produce bile acids, which help in digesting and absorbing dietary fats.
Sources of Cholesterol
Cholesterol comes from two primary sources:
- Endogenous (Produced by the Body): The liver produces most of the cholesterol needed for normal bodily functions.
- Exogenous (From Food): Some cholesterol is obtained through animal-based foods like eggs, dairy products, meat, and shellfish.
Why Cholesterol Levels Matter
While cholesterol is essential, an imbalance in cholesterol levels can lead to health risks, particularly cardiovascular diseases. When too much low-density lipoprotein (LDL), or “bad cholesterol,” circulates in the blood, it can accumulate in artery walls, leading to atherosclerosis (hardening of the arteries). In contrast, high-density lipoprotein (HDL), or “good cholesterol,” helps remove excess cholesterol from the bloodstream, reducing the risk of heart disease and stroke.
Understanding cholesterol and its role in the body is the first step in managing and maintaining a healthy balance for overall well-being.
LDL vs. HDL: The Good and the Bad (Differences and Impact on Health)
Cholesterol is transported through the bloodstream by molecules called lipoproteins. The two primary types of cholesterol—low-density lipoprotein (LDL) and high-density lipoprotein (HDL)—play opposite roles in heart health. Understanding their functions and effects on the body is key to maintaining a healthy cardiovascular system.
What Is LDL (“Bad Cholesterol”)?
Low-Density Lipoprotein (LDL) is often referred to as “bad cholesterol” because high levels can lead to plaque buildup in the arteries. Plaque is a sticky, fatty substance that can harden over time, narrowing the arteries and reducing blood flow. This condition, known as atherosclerosis, significantly increases the risk of:
- Heart attacks (due to blocked arteries supplying the heart)
- Strokes (caused by reduced blood flow to the brain)
- Peripheral artery disease (PAD) (narrowing of blood vessels in the limbs)
What Causes High LDL Cholesterol?
- Diets high in saturated fats, trans fats, and cholesterol-rich foods
- Lack of physical activity
- Excess body weight and obesity
- Genetic conditions such as familial hypercholesterolemia
- Smoking, which lowers HDL and damages blood vessels
- Medical conditions like diabetes and hypothyroidism
Keeping LDL cholesterol levels low is crucial to reducing the risk of cardiovascular disease.
What Is HDL (“Good Cholesterol”)?
High-Density Lipoprotein (HDL) is known as “good cholesterol” because it helps remove excess cholesterol from the bloodstream. HDL carries cholesterol from the arteries back to the liver, where it is broken down and eliminated from the body. This process prevents cholesterol from accumulating in the blood vessels, lowering the risk of heart disease and stroke.
Benefits of High HDL Levels:
- Reduces LDL cholesterol buildup in the arteries
- Lowers the risk of heart disease and stroke
- Has anti-inflammatory and antioxidant properties that protect blood vessels
How to Increase HDL Cholesterol Naturally:
- Regular physical activity (exercise boosts HDL levels)
- Healthy fats (eating nuts, olive oil, fatty fish, and avocados)
- Avoiding smoking (smoking reduces HDL and damages blood vessels)
- Maintaining a healthy weight (excess weight lowers HDL)
The Ideal Cholesterol Balance
For optimal heart health, it’s important to keep LDL levels low and HDL levels high. Doctors typically recommend the following cholesterol levels:
| Cholesterol Type | Optimal Level (mg/dL) |
|---|---|
| LDL (“Bad”) | Less than 100 |
| HDL (“Good”) | 60 or higher |
| Total Cholesterol | Less than 200 |
Maintaining a balanced ratio of LDL and HDL is essential for cardiovascular health. If LDL is too high and HDL is too low, the risk of heart disease increases significantly.
By adopting a heart-healthy diet, regular exercise, and lifestyle changes, you can naturally improve your cholesterol levels and protect your heart
Triglycerides and Their Role (Why They Matter for Heart Health)
Triglycerides are a type of fat (lipid) found in the blood that serve as a major source of energy for the body. While they are essential for normal bodily functions, having high triglyceride levels can increase the risk of heart disease, stroke, and other cardiovascular issues. Understanding what triglycerides are, how they function, and how to maintain healthy levels is crucial for overall heart health.
What Are Triglycerides?
Triglycerides are composed of three fatty acids attached to a glycerol backbone—hence the name “tri-glycerides.” They are stored in fat cells and released for energy when the body needs fuel between meals.
When you eat, excess calories, especially from carbohydrates and fats, are converted into triglycerides and stored in fat cells for later use. If you consistently consume more calories than your body burns, triglyceride levels can rise, increasing the risk of metabolic disorders.
Why Do Triglycerides Matter for Heart Health?
While triglycerides themselves are not a form of cholesterol, they are closely linked to cardiovascular health. High triglyceride levels are often associated with:
- Increased Risk of Atherosclerosis:
- High triglycerides contribute to plaque buildup in the arteries, leading to narrowing and hardening of blood vessels.
- This can restrict blood flow, raising the risk of heart attacks, strokes, and peripheral artery disease (PAD).
- Connection to High LDL and Low HDL:
- High triglyceride levels are often accompanied by low HDL (“good cholesterol”) and high LDL (“bad cholesterol”), which further worsens heart health.
- This dangerous combination increases the likelihood of developing coronary artery disease.
- Association with Metabolic Syndrome:
- Metabolic syndrome is a group of conditions—including high triglycerides, high blood sugar, obesity, high blood pressure, and low HDL cholesterol—that significantly increases the risk of heart disease, diabetes, and stroke.
What Causes High Triglyceride Levels?
Several factors contribute to elevated triglycerides, including:
- Excessive calorie intake: Consuming more calories than your body needs, particularly from sugar, refined carbohydrates, and unhealthy fats.
- Sedentary lifestyle: Lack of physical activity leads to poor fat metabolism, causing triglycerides to rise.
- Obesity: Being overweight, especially with excess belly fat, is strongly linked to high triglycerides.
- Uncontrolled diabetes: High blood sugar levels can increase triglycerides.
- Alcohol consumption: Excess alcohol intake raises triglycerides and damages the liver.
- Medical conditions: Hypothyroidism, kidney disease, and liver disease can contribute to elevated triglycerides.
- Genetics: Some people have a hereditary condition called familial hypertriglyceridemia, which leads to naturally high triglyceride levels.
How to Lower Triglyceride Levels Naturally
Maintaining healthy triglyceride levels (below 150 mg/dL) is crucial for cardiovascular well-being. Here are some proven ways to lower triglycerides:
- Adopt a Heart-Healthy Diet:
- Reduce intake of sugar and refined carbs (e.g., white bread, pastries, soda).
- Eat more healthy fats like omega-3 fatty acids found in salmon, walnuts, flaxseeds, and chia seeds.
- Increase fiber consumption with vegetables, whole grains, and legumes.
- Exercise Regularly:
- Engage in at least 150 minutes of moderate exercise per week (walking, cycling, swimming, etc.).
- Physical activity helps burn excess triglycerides for energy and improves fat metabolism.
- Lose Excess Weight:
- Even a 5–10% weight loss can significantly lower triglycerides.
- Focus on portion control and balanced meals to achieve sustainable weight loss.
- Limit Alcohol Consumption:
- Alcohol is high in calories and sugar, which can spike triglyceride levels.
- Reducing alcohol intake can have an immediate positive impact.
- Manage Underlying Health Conditions:
- If you have diabetes, hypothyroidism, or other metabolic disorders, work with your doctor to manage them effectively.
When to Seek Medical Help
If lifestyle changes aren’t enough to lower triglycerides, doctors may recommend:
- Statins: Primarily used for lowering LDL cholesterol but can also reduce triglycerides.
- Fibrates: Medications that specifically target high triglyceride levels.
- Omega-3 Supplements: High-dose fish oil supplements can lower triglycerides naturally.
- Niacin (Vitamin B3): Can help lower triglycerides but should be taken under medical supervision.
Final Thoughts
While triglycerides play an essential role in energy storage and metabolism, elevated levels pose a significant risk to heart health. By adopting a healthy diet, regular exercise, and lifestyle changes, you can effectively manage your triglyceride levels and reduce the risk of heart disease. Regular blood tests are recommended to monitor triglyceride levels and maintain optimal cardiovascular health.
What’s Considered Normal and What’s Not?
Normal Cholesterol Range (LDL, HDL, and Total Cholesterol Levels)
Maintaining healthy cholesterol levels is essential for heart health and overall well-being. Cholesterol is measured through a lipid panel (cholesterol test), which provides readings for LDL (low-density lipoprotein), HDL (high-density lipoprotein), total cholesterol, and triglycerides. Understanding what these numbers mean can help you assess your risk for heart disease and take steps to improve your health if needed.
What Are the Recommended Cholesterol Levels?
The American Heart Association (AHA) and other health organizations provide guidelines for optimal cholesterol levels to reduce the risk of cardiovascular disease. Below is a general reference for what is considered normal, borderline, and high cholesterol:
| Cholesterol Type | Healthy Level | Borderline | High/Risky Level |
|---|---|---|---|
| LDL (“Bad” Cholesterol) | Less than 100 mg/dL | 100–159 mg/dL | 160 mg/dL or higher |
| HDL (“Good” Cholesterol) | 60 mg/dL or higher | 40–59 mg/dL | Less than 40 mg/dL (men) / Less than 50 mg/dL (women) |
| Total Cholesterol | Less than 200 mg/dL | 200–239 mg/dL | 240 mg/dL or higher |
| Triglycerides | Less than 150 mg/dL | 150–199 mg/dL | 200 mg/dL or higher |
Note: Cholesterol is measured in milligrams per deciliter (mg/dL) of blood.
Each component of your cholesterol profile plays a different role in your cardiovascular health:
LDL (“Bad” Cholesterol) – Why It Matters
LDL (low-density lipoprotein) is often called “bad cholesterol” because high levels contribute to plaque buildup in the arteries, leading to atherosclerosis (narrowing of the arteries). This increases the risk of:
- Heart attacks (blocked coronary arteries)
- Strokes (reduced blood flow to the brain)
- Peripheral artery disease (PAD)
LDL Cholesterol Levels and Risk:
- Optimal: Less than 100 mg/dL (ideal for most adults)
- Near-Optimal: 100–129 mg/dL
- Borderline High: 130–159 mg/dL
- High: 160–189 mg/dL
- Very High: 190 mg/dL or more (increased risk of cardiovascular disease)
Goal: Keep LDL levels low to protect heart health.
HDL (“Good” Cholesterol) – Why It’s Important
HDL (high-density lipoprotein) is known as “good cholesterol” because it helps remove excess cholesterol from the bloodstream and transports it back to the liver for excretion. Higher HDL levels are associated with a lower risk of heart disease and stroke.
HDL Cholesterol Levels and Risk:
- Optimal (Protective): 60 mg/dL or higher (reduces heart disease risk)
- Acceptable: 40–59 mg/dL (moderate risk)
- Low (Risky): Less than 40 mg/dL for men / Less than 50 mg/dL for women (higher risk of heart disease)
Goal: Aim for higher HDL levels to protect against heart disease.
Total Cholesterol – What It Represents
Total cholesterol is the sum of LDL, HDL, and 20% of triglycerides. While total cholesterol provides an overall snapshot of your cholesterol levels, it is important to look at LDL and HDL individually for a clearer understanding of heart disease risk.
Total Cholesterol Levels and Risk:
- Desirable: Less than 200 mg/dL
- Borderline High: 200–239 mg/dL
- High: 240 mg/dL or higher
A high total cholesterol level can be concerning, but it’s important to check LDL and HDL levels separately to get a better picture of your risk.
Why Checking Your Cholesterol Levels Regularly Is Important
Since high cholesterol often has no symptoms, regular blood tests are essential to monitor your levels and take action if needed. The American Heart Association (AHA) recommends:
- Adults aged 20+: Get a lipid profile test every 4–6 years if risk factors are low.
- People with heart disease, diabetes, or high cholesterol history: Get tested annually or as recommended by a doctor.
- Children and teenagers (ages 9–11, and again at 17–21): Screening may be needed if there’s a family history of high cholesterol.
What to Do If Your Cholesterol Levels Are High
If your LDL or total cholesterol is elevated, or your HDL is too low, consider these steps:
- Improve Your Diet:
- Eat more fiber, healthy fats, and omega-3s (found in nuts, seeds, fatty fish, and avocados).
- Reduce saturated and trans fats from processed foods, fried foods, and red meat.
- Exercise Regularly:
- Engage in moderate physical activity (brisk walking, cycling, swimming) for 30 minutes a day, at least 5 times a week.
- Maintain a Healthy Weight:
- Even a small weight loss (5–10% of body weight) can significantly lower LDL and triglyceride levels.
- Quit Smoking and Limit Alcohol:
- Smoking lowers HDL (“good cholesterol”) and increases heart disease risk.
- Excess alcohol raises triglycerides and contributes to cholesterol imbalances.
- Consider Medication If Necessary:
- If lifestyle changes are not enough, statins or other cholesterol-lowering medications may be prescribed by your doctor.
Final Thoughts
Maintaining healthy cholesterol levels is essential for reducing the risk of heart disease, stroke, and other cardiovascular complications. By regularly checking your LDL, HDL, total cholesterol, and triglycerides, you can take proactive steps toward better heart health.
If your cholesterol levels are outside the healthy range, lifestyle changes, dietary improvements, and medical interventions (if needed) can help you get back on track.
Symptoms of High Cholesterol (Why It’s Often Called a ‘Silent’ Condition)
High cholesterol is often referred to as a “silent” condition because it typically does not cause noticeable symptoms. Many people do not realize they have high cholesterol until they undergo a routine blood test or experience a serious cardiovascular event, such as a heart attack or stroke. This is why regular cholesterol screenings are essential for detecting and managing high cholesterol before it leads to severe health complications.
Why Doesn’t High Cholesterol Cause Symptoms?
Cholesterol is a fat-like substance that circulates in the blood. Unlike conditions such as diabetes or high blood pressure, which may produce symptoms like excessive thirst or headaches, high cholesterol does not directly cause physical discomfort. Instead, its effects develop gradually over time, often silently damaging blood vessels and increasing the risk of heart disease.
How High Cholesterol Affects the Body Without Symptoms
Although high cholesterol itself doesn’t cause symptoms, it plays a major role in the development of cardiovascular disease. The long-term consequences of high cholesterol include:
- Atherosclerosis (Plaque Buildup in Arteries)
- Excess LDL (“bad cholesterol”) can stick to artery walls, forming plaques that harden and narrow the arteries.
- This restricts blood flow, increasing the risk of high blood pressure, heart attacks, and strokes.
- Reduced Blood Circulation
- As arteries narrow due to plaque buildup, oxygen-rich blood has a harder time reaching vital organs.
- This can contribute to chest pain (angina), fatigue, dizziness, and cold extremities.
- Increased Risk of Blood Clots
- Plaques can rupture, leading to blood clots that may completely block an artery.
- A blocked artery in the heart can cause a heart attack, while a blocked artery in the brain can lead to a stroke.
Warning Signs of Complications from High Cholesterol
While high cholesterol itself does not cause symptoms, its long-term effects can result in noticeable health problems. Some signs that may indicate serious complications include:
1. Chest Pain or Angina
- A feeling of pressure, tightness, or pain in the chest that occurs when the heart isn’t receiving enough oxygen.
- Usually occurs during physical exertion or stress and goes away with rest.
- Can be an early sign of coronary artery disease (CAD) caused by high cholesterol.
2. Shortness of Breath
- If cholesterol buildup restricts blood flow to the heart and lungs, it can cause breathlessness, especially during exercise or exertion.
- This may indicate blockages in the arteries supplying the heart.
3. Fatigue and Weakness
- Inadequate blood flow to muscles and organs can cause persistent fatigue and weakness.
- Can be linked to poor circulation, reduced oxygen delivery, or an undiagnosed heart condition.
4. Numbness or Coldness in Extremities
- Narrowed arteries can reduce blood flow to the legs, feet, hands, and arms.
- This may cause cold sensations, tingling, or numbness, particularly in the feet and toes.
- Can be a sign of peripheral artery disease (PAD), a condition caused by high cholesterol and plaque buildup in the arteries outside the heart.
5. High Blood Pressure
- High cholesterol and atherosclerosis can lead to elevated blood pressure because the heart has to work harder to pump blood through narrowed arteries.
- Over time, hypertension increases the risk of heart attacks and strokes.
6. Sudden Stroke or Heart Attack Symptoms
- In some cases, high cholesterol is only diagnosed after a person experiences a stroke or heart attack.
- Signs of a heart attack may include:
- Chest pain or discomfort (often radiating to the left arm, jaw, or back)
- Shortness of breath
- Nausea or dizziness
- Cold sweats
- Signs of a stroke may include:
- Sudden numbness or weakness (especially on one side of the body)
- Confusion, trouble speaking, or difficulty understanding speech
- Vision problems or loss of coordination
Emergency Tip: If you or someone else experiences stroke or heart attack symptoms, seek immediate medical attention.
How to Detect High Cholesterol Early
Since high cholesterol doesn’t cause symptoms, the only way to diagnose it early is through a blood test.
Lipid Panel (Cholesterol Test) Recommendations
- Adults (20+ years old) → Get tested at least every 4–6 years if risk factors are low.
- People with heart disease, diabetes, or a family history of high cholesterol → Get tested annually or as recommended by a doctor.
- Children and teens with a family history of high cholesterol → Screening may be necessary starting at ages 9–11 and again at 17–21.
Proactive health care is key: Regular cholesterol tests help you catch high cholesterol before it leads to life-threatening conditions.
Take Action: How to Prevent and Manage High Cholesterol
Even though high cholesterol is silent, you can actively prevent and control it by making lifestyle changes and, if necessary, using medication.
✔ Eat a Heart-Healthy Diet → Focus on fiber-rich foods (oats, legumes, vegetables), healthy fats (avocados, nuts, olive oil), and omega-3 sources (fatty fish). Avoid trans fats and excessive saturated fats.
✔ Exercise Regularly → Engage in at least 30 minutes of moderate activity most days (walking, cycling, swimming).
✔ Maintain a Healthy Weight → Losing just 5–10% of body weight can significantly lower LDL cholesterol levels.
✔ Quit Smoking → Smoking lowers HDL (good cholesterol) and worsens artery damage.
✔ Limit Alcohol Consumption → Excess alcohol increases triglycerides, contributing to heart disease risk.
✔ Manage Stress → Chronic stress can lead to poor eating habits and increased cholesterol levels. Practice relaxation techniques like meditation or deep breathing.
✔ Follow Your Doctor’s Advice → If lifestyle changes aren’t enough, medications like statins may be recommended to help lower cholesterol.
Final Thoughts
High cholesterol is a silent but serious condition that can go unnoticed for years. Without symptoms, it quietly increases the risk of heart disease, stroke, and other cardiovascular complications. Because of this, regular cholesterol screenings are crucial for early detection and prevention.
By making healthy lifestyle choices, monitoring your cholesterol levels, and seeking medical guidance when necessary, you can reduce your risk and protect your heart health for the long term.
Causes of High Cholesterol (Diet, Lifestyle, Genetics, and Medical Conditions)
High cholesterol can result from a combination of lifestyle choices, genetic factors, and underlying medical conditions. Understanding these causes can help individuals take proactive steps to reduce cholesterol levels and lower the risk of heart disease.
1. Diet: The Food You Eat Matters
Your diet plays a crucial role in determining cholesterol levels. Certain foods can increase LDL (bad cholesterol) while others can help boost HDL (good cholesterol).
Foods That Raise LDL (Bad Cholesterol)
- Saturated Fats: Found in red meat, full-fat dairy products, butter, and tropical oils (coconut and palm oil).
- Trans Fats: Common in processed foods, margarine, fried fast food, and commercially baked goods.
- Excessive Sugar and Refined Carbs: Sugary drinks, white bread, pastries, and processed snacks contribute to high triglycerides, which are linked to high cholesterol.
- Processed and Fast Foods: High in unhealthy fats, sodium, and preservatives that negatively impact heart health.
Foods That Help Lower Cholesterol
- Healthy Fats: Found in olive oil, avocados, and fatty fish like salmon.
- Soluble Fiber: Oats, legumes, fruits, and vegetables help reduce cholesterol absorption in the bloodstream.
- Nuts and Seeds: Almonds, walnuts, flaxseeds, and chia seeds contain heart-healthy fats and fiber.
- Plant Sterols and Stanols: Found in fortified foods like certain spreads, juices, and cereals, these compounds help block cholesterol absorption.
📌 Key Takeaway: Eating a heart-healthy diet that is low in saturated fats and processed foods while rich in fiber and healthy fats can help manage cholesterol levels.
2. Lifestyle: Daily Habits That Affect Cholesterol
Your daily habits and choices can significantly influence cholesterol levels. An unhealthy lifestyle can lead to high cholesterol, increasing the risk of heart disease over time.
Lifestyle Factors That Raise Cholesterol
- Lack of Physical Activity:
- Sedentary behavior lowers HDL (good cholesterol) and raises LDL (bad cholesterol).
- Regular exercise helps the body use cholesterol efficiently and improve heart health.
- Smoking and Tobacco Use:
- Lowers HDL (good cholesterol), making it harder for the body to remove LDL from the blood.
- Damages blood vessels, increasing the risk of plaque buildup and atherosclerosis.
- Excessive Alcohol Consumption:
- Increases triglycerides, contributing to high cholesterol and heart disease risk.
- Heavy drinking can also raise blood pressure and cause liver damage.
- Being Overweight or Obese:
- Excess body weight, especially around the abdomen, raises LDL and triglycerides while lowering HDL.
- Losing even 5–10% of body weight can help improve cholesterol levels.
📌 Key Takeaway: Maintaining an active lifestyle, quitting smoking, reducing alcohol intake, and achieving a healthy weight can positively impact cholesterol levels.
3. Genetics: Family History and Inherited Conditions
For some people, high cholesterol is not just a result of lifestyle choices but is influenced by genetics. This is known as familial hypercholesterolemia (FH)—a condition where the body struggles to regulate cholesterol levels due to inherited genetic mutations.
How Genetics Influence Cholesterol
- If one or both parents have high cholesterol, there’s a greater chance of inheriting high cholesterol levels.
- People with familial hypercholesterolemia (FH) may develop dangerously high LDL cholesterol levels at a young age.
- Some individuals have a genetic predisposition that makes their bodies produce too much cholesterol or struggle to remove excess cholesterol from the blood.
Who Should Be Concerned About Genetic High Cholesterol?
- If multiple family members have a history of heart disease, strokes, or high cholesterol, genetic testing or early cholesterol screening is recommended.
- Children with a family history of high cholesterol may need screening as early as 9–11 years old.
- Those diagnosed with FH may require cholesterol-lowering medications (statins or PCSK9 inhibitors) in addition to lifestyle changes.
📌 Key Takeaway: If high cholesterol runs in your family, regular testing and early intervention are essential to prevent heart disease.
4. Medical Conditions That Contribute to High Cholesterol
Certain health conditions can cause abnormal cholesterol levels, even in individuals who maintain a healthy diet and lifestyle.
Common Medical Conditions That Increase Cholesterol
- Hypothyroidism (Underactive Thyroid)
- Slows down metabolism, leading to higher LDL cholesterol levels.
- Treating the thyroid disorder can help regulate cholesterol.
- Diabetes
- High blood sugar damages blood vessels and increases LDL while lowering HDL.
- People with diabetes have a higher risk of heart disease due to poor cholesterol balance.
- Liver Disease
- The liver plays a key role in cholesterol production and metabolism.
- Liver conditions like fatty liver disease or cirrhosis can disrupt cholesterol levels.
- Kidney Disease
- Can cause an increase in LDL and triglycerides due to poor filtration and metabolism of fats.
- Polycystic Ovary Syndrome (PCOS)
- Hormonal imbalances associated with PCOS can lead to elevated LDL and lower HDL levels.
- Cushing’s Syndrome
- A condition caused by excess cortisol production, leading to high cholesterol and increased cardiovascular risk.
- Menopause and Hormonal Changes
- Postmenopausal women often experience a natural increase in LDL and a decrease in HDL due to lower estrogen levels.
📌 Key Takeaway: If you have an underlying medical condition, working with a healthcare provider to manage it can help keep cholesterol levels in check.
How to Reduce High Cholesterol Caused by These Factors
Regardless of the cause, high cholesterol can be managed with the right approach.
✅ Improve Diet: Focus on fiber-rich foods, healthy fats, and whole foods while avoiding processed and fried foods.
✅ Exercise Regularly: Engage in at least 150 minutes of moderate exercise per week to boost HDL and reduce LDL.
✅ Lose Excess Weight: Even a small weight loss can significantly lower cholesterol and improve heart health.
✅ Quit Smoking: Eliminating tobacco use can raise HDL and improve blood circulation.
✅ Limit Alcohol: Moderate consumption or avoiding alcohol can prevent spikes in cholesterol levels.
✅ Manage Stress: Chronic stress can contribute to poor lifestyle choices that raise cholesterol—practicing mindfulness, yoga, or deep breathing can help.
✅ Take Medications if Necessary: Some individuals may need statins, PCSK9 inhibitors, or other cholesterol-lowering drugs if lifestyle changes aren’t enough.
Final Thoughts
High cholesterol can be caused by unhealthy lifestyle choices, genetics, and medical conditions. While some factors, like genetics, cannot be changed, lifestyle modifications and medical treatments can help manage cholesterol effectively.
By taking proactive steps to monitor and control cholesterol, individuals can reduce their risk of heart disease, stroke, and other cardiovascular complications, leading to a longer and healthier life.
How to Improve Your Cholesterol Levels Naturally

Cholesterol-Lowering Foods (Best Diet Choices: Fiber, Omega-3s, Healthy Fats)
Diet plays a crucial role in managing cholesterol levels. The right foods can help lower LDL (bad cholesterol), boost HDL (good cholesterol), and improve overall heart health. Incorporating fiber-rich foods, omega-3 fatty acids, and healthy fats into your diet can significantly impact cholesterol levels and reduce the risk of cardiovascular diseases.
1. Fiber: The Heart-Healthy Nutrient
Fiber, particularly soluble fiber, helps lower cholesterol by binding to cholesterol molecules in the digestive tract and preventing their absorption into the bloodstream. Instead, the cholesterol is eliminated through waste.
Best High-Fiber Foods for Lowering Cholesterol
✅ Oats and Barley – Contain beta-glucan, a type of soluble fiber that helps reduce LDL cholesterol.
✅ Legumes (Lentils, Chickpeas, and Beans) – High in fiber and protein, they slow down cholesterol absorption.
✅ Fruits (Apples, Pears, and Berries) – Rich in pectin, a soluble fiber known to lower LDL cholesterol.
✅ Vegetables (Carrots, Brussels Sprouts, and Sweet Potatoes) – Excellent sources of fiber and antioxidants.
✅ Flaxseeds and Chia Seeds – Packed with fiber and omega-3s, aiding cholesterol management.
📌 Tip: Aim for at least 25–30 grams of fiber per day to support heart health and cholesterol control.
2. Omega-3 Fatty Acids: The Heart’s Best Friend
Omega-3 fatty acids are essential fats that help lower triglycerides, reduce inflammation, and increase HDL (good cholesterol) levels. Unlike saturated fats, they do not raise LDL cholesterol and are beneficial for overall cardiovascular health.
Best Omega-3-Rich Foods
🐟 Fatty Fish (Salmon, Mackerel, Sardines, and Tuna) – Rich in EPA and DHA, which protect the heart.
🌰 Walnuts – A great plant-based source of omega-3s that supports lower cholesterol levels.
🥑 Flaxseeds and Chia Seeds – Provide ALA, a plant-based omega-3 that contributes to heart health.
🥜 Algal Oil and Seaweed – Ideal omega-3 sources for vegetarians and vegans.
📌 Tip: Aim to eat at least two servings of fatty fish per week or take an omega-3 supplement if needed.
3. Healthy Fats: Replacing the Bad with the Good
Not all fats are bad! While saturated and trans fats can raise LDL cholesterol, unsaturated fats (monounsaturated and polyunsaturated fats) help improve cholesterol levels and reduce the risk of heart disease.
Best Healthy Fat Sources for Lowering Cholesterol
🥑 Avocados – High in monounsaturated fats, which help lower LDL while maintaining HDL levels.
🥜 Nuts (Almonds, Walnuts, and Cashews) – Contain heart-healthy fats, fiber, and plant sterols that lower cholesterol.
🫒 Olive Oil – A key component of the Mediterranean diet, olive oil is rich in antioxidants and healthy fats.
🌻 Seeds (Sunflower, Flax, and Pumpkin Seeds) – Provide healthy fats and fiber for cholesterol control.
🌰 Coconut (in Moderation) – While it contains saturated fats, some research suggests that coconut in moderation may not negatively impact heart health.
📌 Tip: Replace butter and processed vegetable oils with olive oil, avocado oil, or nut-based spreads for healthier fat intake.
4. Plant-Based Cholesterol Blockers: Sterols and Stanols
Certain plant-based compounds, called sterols and stanols, mimic cholesterol’s structure and compete for absorption in the intestines. This competition prevents actual cholesterol from entering the bloodstream, reducing LDL levels naturally.
Best Sources of Sterols and Stanols
🥛 Fortified Foods (Orange Juice, Yogurt, and Margarines) – Some brands add plant sterols to help lower cholesterol.
🌰 Nuts and Seeds – Naturally contain sterols that contribute to cholesterol reduction.
🥬 Vegetables (Broccoli, Cauliflower, and Brussels Sprouts) – Provide a combination of fiber and sterols.
📌 Tip: Consuming 2 grams of plant sterols daily can lower LDL cholesterol by up to 10%.
5. Foods to Avoid (Cholesterol-Raising Culprits)
While adding cholesterol-lowering foods to your diet is beneficial, it’s equally important to reduce or eliminate foods that can raise LDL cholesterol and triglycerides.
🚫 Processed and Fried Foods – High in trans fats, which raise LDL and lower HDL.
🚫 Red and Processed Meats – Contain saturated fats and cholesterol that can contribute to plaque buildup.
🚫 Full-Fat Dairy Products – Butter, cream, and cheese can increase cholesterol levels if consumed excessively.
🚫 Sugary Beverages and Sweets – Excess sugar contributes to high triglycerides, impacting cholesterol balance.
🚫 Fast Food and Packaged Snacks – Loaded with unhealthy fats, preservatives, and hidden sugars.
📌 Tip: Read food labels carefully and opt for whole, unprocessed foods whenever possible.
Final Thoughts
Eating the right foods can dramatically improve cholesterol levels and lower the risk of heart disease. By incorporating fiber-rich foods, omega-3 fatty acids, and healthy fats, and avoiding unhealthy dietary choices, you can naturally regulate cholesterol and support heart health.
✅ Increase Fiber Intake – Oats, fruits, vegetables, and legumes.
✅ Consume Omega-3s – Fatty fish, walnuts, and flaxseeds.
✅ Choose Healthy Fats – Avocados, nuts, olive oil.
✅ Add Plant Sterols – Fortified foods, nuts, and vegetables.
✅ Reduce Unhealthy Fats and Sugars – Limit processed, fried, and sugary foods.
By making smart dietary changes, you can take control of your cholesterol and enjoy a healthier, heart-friendly lifestyle.
Exercise and Lifestyle Changes (How Physical Activity Helps Manage Cholesterol)
Regular physical activity is one of the most effective ways to manage cholesterol levels and promote heart health. Exercise not only helps reduce LDL (bad cholesterol) but also increases HDL (good cholesterol), improves circulation, and supports overall cardiovascular function. A well-balanced lifestyle that includes physical activity, stress management, and healthy habits can significantly contribute to better cholesterol levels and a lower risk of heart disease.
1. How Exercise Lowers LDL (Bad Cholesterol)
LDL cholesterol contributes to plaque buildup in the arteries, increasing the risk of heart disease and stroke. Exercise helps reduce LDL levels in several ways:
- Enhancing Enzyme Activity: Physical activity stimulates enzymes that help move LDL from the blood into the liver, where it is broken down and eliminated from the body.
- Burning Excess Fat: Being overweight or obese is associated with higher LDL levels. Regular exercise helps with weight loss and fat metabolism, reducing LDL cholesterol.
- Reducing Inflammation: Chronic inflammation contributes to cholesterol buildup in arteries. Exercise lowers inflammation markers, improving blood vessel function and reducing the risk of plaque formation.
2. How Exercise Increases HDL (Good Cholesterol)
HDL cholesterol acts as a protective agent by transporting excess cholesterol from the bloodstream to the liver for removal. Higher levels of HDL are linked to a reduced risk of cardiovascular disease. Exercise increases HDL levels by:
- Boosting Lipoprotein Metabolism: Physical activity improves the efficiency of HDL in removing LDL from the arteries.
- Improving Insulin Sensitivity: Exercise helps regulate blood sugar levels, which in turn supports better lipid balance and higher HDL levels.
- Promoting Fat Utilization: Regular workouts encourage the body to use fat for energy, enhancing HDL function and reducing unhealthy fat accumulation.
3. Best Types of Exercise for Managing Cholesterol
A combination of aerobic, resistance, and flexibility exercises provides the best results for cholesterol management and overall heart health.
- Aerobic Exercise (Cardio): Activities like brisk walking, jogging, cycling, swimming, and dancing help lower LDL cholesterol and improve heart function. Aim for at least 150 minutes of moderate-intensity or 75 minutes of high-intensity aerobic exercise per week.
- Strength Training (Resistance Exercises): Lifting weights, bodyweight exercises (push-ups, squats, lunges), and resistance band workouts help build muscle and improve metabolic function, contributing to better cholesterol levels. Strength training should be performed at least two days per week.
- High-Intensity Interval Training (HIIT): Short bursts of intense exercise followed by rest periods have been shown to significantly improve cholesterol profiles and cardiovascular health in a shorter time compared to traditional exercise.
- Flexibility and Stress-Relieving Activities: Yoga, Pilates, and stretching exercises may not directly lower cholesterol, but they help reduce stress, which is a contributing factor to high cholesterol and heart disease.
4. Lifestyle Changes That Support Healthy Cholesterol Levels
In addition to exercise, adopting a heart-healthy lifestyle can further enhance cholesterol management and prevent complications.
- Maintain a Healthy Weight: Excess weight contributes to higher LDL and triglyceride levels. Losing even 5-10% of body weight can significantly improve cholesterol levels.
- Quit Smoking: Smoking lowers HDL cholesterol and damages blood vessels, increasing the risk of heart disease. Quitting smoking can lead to noticeable improvements in HDL levels within weeks.
- Limit Alcohol Consumption: Excessive alcohol intake can raise triglycerides and contribute to weight gain. If consumed, it should be done in moderation—one drink per day for women and two for men.
- Manage Stress: Chronic stress can negatively impact cholesterol levels by promoting unhealthy eating habits, increasing inflammation, and disrupting metabolic functions. Techniques such as meditation, deep breathing, and spending time in nature can help lower stress levels.
- Get Quality Sleep: Poor sleep patterns are linked to metabolic disorders and high cholesterol. Aim for 7-9 hours of restful sleep per night to support heart health and overall well-being.
Making exercise and lifestyle changes a consistent part of daily life can significantly improve cholesterol levels, reduce the risk of heart disease, and enhance overall health.
The Role of Supplements (Do Omega-3, Niacin, or Plant Sterols Help?)
Supplements can play a supportive role in managing cholesterol levels, especially for individuals who struggle to maintain optimal levels through diet and lifestyle alone. While they should not replace a balanced diet and regular exercise, certain supplements, such as omega-3 fatty acids, niacin (vitamin B3), and plant sterols, have been shown to positively influence cholesterol levels and overall heart health.
1. Omega-3 Fatty Acids: Heart-Healthy Fats for Cholesterol Management
Omega-3 fatty acids are essential fats found primarily in fatty fish, flaxseeds, and walnuts. They are known for their anti-inflammatory properties and cardiovascular benefits, particularly in reducing triglycerides.
How Omega-3s Affect Cholesterol and Heart Health
- Lower Triglycerides: Omega-3s can significantly reduce triglyceride levels, a type of fat in the blood that contributes to heart disease.
- Increase HDL (Good Cholesterol): While they may not directly lower LDL, omega-3s can help raise HDL levels, improving overall cholesterol balance.
- Reduce Inflammation and Blood Clotting: Chronic inflammation contributes to heart disease, and omega-3s help counteract this effect. They also improve blood flow and reduce the risk of clot formation.
Best Omega-3 Supplements for Cholesterol Control
- Fish Oil Supplements: Rich in EPA (eicosapentaenoic acid) and DHA (docosahexaenoic acid), fish oil is the most studied form of omega-3 for heart health.
- Krill Oil: A source of omega-3s that may be more easily absorbed by the body.
- Algal Oil: A plant-based omega-3 supplement derived from algae, ideal for vegetarians and vegans.
Recommended Dosage
The American Heart Association (AHA) recommends 1,000–4,000 mg of EPA and DHA per day for those with high triglycerides, but it’s important to consult a doctor before taking high doses.
2. Niacin (Vitamin B3): A Powerful Cholesterol-Lowering Vitamin
Niacin, also known as vitamin B3, has been used for decades to help manage cholesterol levels. It is known for its ability to raise HDL cholesterol and lower LDL and triglycerides.
How Niacin Helps with Cholesterol
- Increases HDL (Good Cholesterol): Niacin can raise HDL levels by up to 35%, which helps remove excess LDL from the bloodstream.
- Lowers LDL and Triglycerides: Niacin reduces the liver’s ability to produce LDL cholesterol and triglycerides.
- Improves Arterial Health: Niacin helps widen blood vessels, improving circulation and reducing plaque buildup.
Potential Side Effects and Considerations
While niacin is effective, it can cause flushing, which is a temporary redness and warmth of the skin. Other potential side effects include:
- Liver damage (at high doses)
- Gastrointestinal issues
- Increased blood sugar levels (important for diabetics)
Recommended Dosage
For cholesterol management, niacin is usually taken in doses of 500–2,000 mg per day under medical supervision. Prescription niacin is preferred over over-the-counter versions, as it is better regulated and less likely to cause severe side effects.
3. Plant Sterols and Stanols: Natural Cholesterol Blockers
Plant sterols and stanols are naturally occurring compounds found in plants that mimic cholesterol and block its absorption in the intestines. They are particularly effective at lowering LDL cholesterol without affecting HDL or triglycerides.
How Plant Sterols and Stanols Work
- Block Cholesterol Absorption: Because plant sterols are structurally similar to cholesterol, they compete for absorption in the digestive system, reducing the amount of LDL that enters the bloodstream.
- Lower LDL Levels: Studies show that consuming 2 grams of plant sterols per day can lower LDL cholesterol by 5-15%.
Best Sources of Plant Sterols and Stanols
- Fortified Foods: Some brands add plant sterols to products like margarine, orange juice, and yogurt.
- Nuts and Seeds: Natural sources of sterols that also provide healthy fats.
- Vegetables and Whole Grains: While present in small amounts, they contribute to daily intake.
Recommended Dosage
For effective cholesterol reduction, aim for 1.5–2.5 grams of plant sterols or stanols daily, either from food or supplements.
Other Cholesterol-Lowering Supplements Worth Considering

Soluble Fiber (Psyllium Husk and Beta-Glucans)
- Found in oats, barley, and fiber supplements like psyllium husk.
- Helps reduce LDL cholesterol by binding to it in the digestive tract and eliminating it.
- Recommended intake: 5–10 grams per day for cholesterol-lowering effects.
Coenzyme Q10 (CoQ10)
- An antioxidant that may help reduce LDL oxidation and support heart health.
- Some studies suggest CoQ10 can help counteract the muscle pain caused by statin medications.
- Recommended intake: 100–200 mg per day.
Red Yeast Rice
- Contains naturally occurring statins that help lower cholesterol.
- Can be effective but should be used cautiously due to potential liver and muscle side effects.
- Recommended intake: 600–1,200 mg per day under medical supervision.
Key Considerations Before Taking Supplements
- Consult a Doctor: Some cholesterol-lowering supplements can interact with medications, especially statins and blood thinners.
- Lifestyle Still Matters: Supplements work best when combined with a healthy diet and exercise.
- Quality Matters: Choose high-quality, third-party tested supplements to ensure safety and effectiveness.
Supplements like omega-3 fatty acids, niacin, and plant sterols can be valuable tools in cholesterol management, but they should be used alongside other lifestyle changes for the best results.
Medical Interventions and When to Seek Help
When to Get Tested (How Often You Should Check Cholesterol Levels)
Regular cholesterol testing is crucial for maintaining heart health and preventing serious conditions like heart disease and stroke. Since high cholesterol often has no noticeable symptoms, routine screening is the only way to detect unhealthy cholesterol levels early. The frequency of cholesterol testing depends on factors like age, health status, family history, and existing medical conditions.
1. General Guidelines for Cholesterol Testing
The American Heart Association (AHA) and the Centers for Disease Control and Prevention (CDC) recommend the following testing schedules based on age and risk factors:
For Adults:
- Ages 20–39: Get tested at least once every 4–6 years if you have no risk factors.
- Ages 40 and older: Get tested more frequently, ideally every 1–2 years, especially if you have risk factors like obesity, smoking, or high blood pressure.
For High-Risk Individuals:
- If you have a family history of high cholesterol or heart disease, testing may be recommended every year or more frequently.
- If you have diabetes, high blood pressure, or are overweight, annual cholesterol testing is advised.
- If you take cholesterol-lowering medications (statins or supplements), regular monitoring helps assess progress and medication effectiveness.
For Children and Adolescents:
- Ages 9–11: One baseline cholesterol test is recommended.
- Ages 17–21: Another screening should be done before adulthood.
- Earlier testing (as young as age 2) may be necessary if a child has a strong family history of high cholesterol or early heart disease.
2. What Does a Cholesterol Test Involve?
A cholesterol test, also known as a lipid panel or lipid profile, is a simple blood test that measures different types of fats in the blood. The test results typically include:
- Total Cholesterol: A combination of LDL, HDL, and other lipid components.
- LDL (Low-Density Lipoprotein) Cholesterol: The “bad” cholesterol that can lead to plaque buildup in arteries.
- HDL (High-Density Lipoprotein) Cholesterol: The “good” cholesterol that helps remove excess LDL from the bloodstream.
- Triglycerides: A type of fat that, when elevated, increases the risk of heart disease.
Fasting vs. Non-Fasting Cholesterol Test
- In most cases, fasting for 9–12 hours before the test (no food or drink except water) provides the most accurate triglyceride readings.
- However, non-fasting cholesterol tests are now considered acceptable for most routine screenings.
3. When to Test More Frequently
Certain medical conditions and lifestyle factors may require more frequent cholesterol checks, such as:
- Obesity or Poor Diet: If you consume high amounts of saturated fats and processed foods, cholesterol levels may rise quickly.
- Sedentary Lifestyle: Lack of exercise contributes to higher LDL and lower HDL cholesterol.
- Diabetes or Insulin Resistance: Diabetes increases the risk of high cholesterol, requiring annual or semi-annual monitoring.
- Smoking and Alcohol Consumption: Smoking lowers HDL levels, while excessive alcohol intake raises triglycerides, increasing the need for monitoring.
- History of Heart Attack or Stroke: If you have experienced cardiovascular disease, your doctor may recommend testing every 3–6 months to ensure cholesterol is under control.
4. Monitoring Cholesterol After Starting Treatment
If you are on cholesterol-lowering medications (such as statins, fibrates, or PCSK9 inhibitors) or making significant lifestyle changes to improve cholesterol levels, follow-up testing is needed:
- Every 1–3 months after starting a new medication or dietary change to track effectiveness.
- Every 6 months to a year once cholesterol is well managed.
Regular cholesterol testing ensures early detection of imbalances and allows for timely interventions, reducing the risk of heart-related complications.
Medications for High Cholesterol (Statins and Other Treatment Options)
When lifestyle changes like diet and exercise are not enough to bring cholesterol levels within a healthy range, doctors may prescribe medications to help manage high cholesterol. Several types of cholesterol-lowering drugs are available, each working differently to reduce LDL (“bad”) cholesterol, raise HDL (“good”) cholesterol, or lower triglycerides.
The most commonly prescribed medications are statins, but there are also other drug classes that can be used alone or in combination, depending on a patient’s specific cholesterol profile and risk factors for heart disease.
1. Statins: The First-Line Treatment for High Cholesterol
What Are Statins?
Statins are the most widely prescribed cholesterol-lowering drugs. They work by blocking an enzyme in the liver (HMG-CoA reductase) that helps produce cholesterol. This results in lower LDL cholesterol and total cholesterol levels while slightly increasing HDL cholesterol.
Benefits of Statins
- Reduce LDL cholesterol by 30–50%
- Lower the risk of heart attack and stroke
- Help stabilize plaque buildup in arteries, preventing rupture
- Have anti-inflammatory effects that improve overall heart health
Common Statin Medications
- Atorvastatin (Lipitor) – One of the most potent statins, used for high-risk patients.
- Rosuvastatin (Crestor) – Another strong statin with high LDL-lowering ability.
- Simvastatin (Zocor) – A moderate-intensity statin.
- Pravastatin (Pravachol) & Lovastatin (Mevacor) – Milder statins, often used for patients with moderate cholesterol elevation.
Potential Side Effects of Statins
While statins are generally well-tolerated, some people experience side effects, including:
- Muscle pain or weakness (myopathy)
- Liver enzyme elevation (requires occasional liver function monitoring)
- Increased blood sugar levels, which may slightly raise the risk of diabetes
- Digestive issues, such as nausea or constipation
In rare cases, statins can cause rhabdomyolysis, a serious muscle breakdown condition, but this is extremely uncommon.
2. Ezetimibe (Zetia): Blocking Cholesterol Absorption
Ezetimibe is often prescribed for people who cannot tolerate statins or need additional cholesterol reduction.
How It Works
Instead of blocking cholesterol production like statins, ezetimibe prevents cholesterol absorption in the intestines, reducing LDL levels by 15–25%.
When It’s Used
- As an add-on therapy to statins for further LDL reduction
- For statin-intolerant patients who need an alternative cholesterol-lowering option
Common Side Effects
- Mild digestive issues (diarrhea, stomach pain)
- Fatigue or muscle weakness (rare)
3. PCSK9 Inhibitors: Advanced Therapy for High-Risk Patients
PCSK9 inhibitors are a newer class of cholesterol-lowering drugs that provide dramatic LDL reduction, especially for individuals with genetic high cholesterol (familial hypercholesterolemia) or those at high cardiovascular risk.
How They Work
These drugs block the PCSK9 protein, which allows the liver to remove more LDL cholesterol from the bloodstream. They are injected every 2–4 weeks and can reduce LDL cholesterol by 50–60%.
Common PCSK9 Inhibitors
- Alirocumab (Praluent)
- Evolocumab (Repatha)
Who Should Consider PCSK9 Inhibitors?
- People with genetically high cholesterol that doesn’t respond to statins
- Individuals with severe heart disease needing aggressive LDL reduction
- Statin-intolerant patients requiring an alternative
Potential Downsides
- High cost (these medications are expensive)
- Injection requirement rather than an oral pill
- Possible mild injection-site reactions
4. Bile Acid Sequestrants: Binding Cholesterol in the Gut
Bile acid sequestrants lower cholesterol by binding to bile acids in the intestines, preventing the body from absorbing cholesterol. The liver then has to use up more cholesterol to make bile, effectively reducing LDL levels.
Common Medications in This Class
- Cholestyramine (Questran)
- Colestipol (Colestid)
- Colesevelam (Welchol)
Who Can Benefit?
- People who cannot take statins due to side effects
- Those with mild to moderate LDL elevation
Side Effects
- Bloating, gas, and constipation (since they affect digestion)
- May interfere with the absorption of certain vitamins and medications
5. Fibrates: Targeting High Triglycerides
Fibrates are mainly used for patients with high triglycerides rather than high LDL cholesterol.
Common Fibrate Medications
- Fenofibrate (Tricor, Lipofen)
- Gemfibrozil (Lopid)
How They Work
Fibrates increase the breakdown of triglycerides in the blood while also boosting HDL levels. They are particularly useful for:
- People with triglycerides above 500 mg/dL
- Diabetics with mixed lipid disorders
Side Effects
- Potential liver function changes
- Increased risk of gallstones
- Muscle pain (especially when combined with statins)
6. Niacin (Vitamin B3): Boosting HDL and Lowering LDL
Niacin, also known as vitamin B3, was once widely used to raise HDL cholesterol and lower triglycerides. However, due to its side effects and limited effectiveness, it is now used less frequently.
Effects on Cholesterol
- Increases HDL (good cholesterol) by 20–35%
- Lowers triglycerides
- Slightly reduces LDL cholesterol
Downsides of Niacin
- Flushing (redness and warmth of the skin)
- Liver toxicity risk at high doses
- Possible worsening of blood sugar control in diabetics
Because of these side effects, niacin is usually not the first choice and is only recommended when other treatments fail.
7. Combination Therapy: Using Multiple Drugs for Better Results
Some individuals require a combination of medications to achieve their cholesterol goals, especially if they have very high LDL, high triglycerides, or statin intolerance.
Common Combinations
- Statins + Ezetimibe – Reduces cholesterol production and absorption.
- Statins + PCSK9 Inhibitors – Provides an aggressive LDL-lowering effect.
- Fibrates + Statins – Used cautiously to manage both high triglycerides and LDL.
Key Takeaways
- Statins are the most effective and commonly prescribed cholesterol-lowering medications.
- Ezetimibe helps block cholesterol absorption and is often used with statins.
- PCSK9 inhibitors offer powerful LDL reduction for high-risk patients but are costly.
- Fibrates and bile acid sequestrants serve specialized roles, particularly for high triglycerides or statin intolerance.
- Niacin is less commonly used due to its side effects.
- Regular cholesterol monitoring is essential to track medication effectiveness and adjust treatment as needed.
Cholesterol medications are most effective when combined with a healthy lifestyle, including a balanced diet, regular exercise, and weight management. Always consult a doctor before starting or changing any cholesterol treatment plan.
Managing Risks for Heart Disease (Preventing Complications Like Atherosclerosis)
High cholesterol is one of the major risk factors for heart disease, particularly because it contributes to atherosclerosis, a condition in which fatty deposits (plaque) build up inside the arteries. Over time, this buildup narrows and hardens the arteries, restricting blood flow and increasing the risk of heart attacks, strokes, and other cardiovascular problems. Managing cholesterol levels effectively can prevent or slow down the progression of atherosclerosis, reducing the chances of life-threatening complications.
1. Understanding Atherosclerosis: How It Develops
Atherosclerosis is a gradual process that can start early in life and worsen over time if left unchecked. It occurs in the following stages:
- Cholesterol Buildup – High levels of LDL (bad) cholesterol lead to cholesterol deposits inside the artery walls.
- Inflammation and Immune Response – The immune system detects these deposits as a problem, sending white blood cells (macrophages) to fight them, leading to further inflammation.
- Plaque Formation – Over time, a fatty plaque forms, narrowing the arteries and reducing blood flow.
- Artery Hardening (Calcification) – Calcium deposits make the arteries stiff and less flexible.
- Complications – If a plaque ruptures, it can cause a blood clot, potentially leading to a heart attack or stroke.
Since atherosclerosis progresses silently, many people are unaware they have it until they experience a cardiovascular event. That’s why proactive risk management is critical.
2. Key Risk Factors for Heart Disease
Managing heart disease risk starts with understanding what contributes to atherosclerosis. Some factors are modifiable, meaning you can take steps to change them, while others, like age and genetics, are beyond control.
Modifiable Risk Factors (Things You Can Change):
- High LDL (“bad”) cholesterol – Excess LDL contributes to plaque formation.
- Low HDL (“good”) cholesterol – HDL helps remove excess LDL from the bloodstream.
- High blood pressure (hypertension) – Puts extra strain on the arteries, making them more prone to damage.
- Smoking – Damages the arteries, lowers HDL cholesterol, and increases clot formation.
- Obesity – Especially excess abdominal fat, is linked to high cholesterol and inflammation.
- Sedentary lifestyle – Lack of exercise can lead to higher cholesterol and poor circulation.
- Unhealthy diet – Diets high in saturated fats, trans fats, and processed sugars contribute to high cholesterol and inflammation.
- Diabetes and insulin resistance – High blood sugar damages blood vessels and raises cholesterol levels.
- Chronic stress – Triggers the release of stress hormones, which may increase blood pressure and cholesterol.
Non-Modifiable Risk Factors (Things You Can’t Change):
- Age – Risk increases as you get older.
- Family history – A genetic predisposition to high cholesterol or early heart disease raises the risk.
- Gender – Men tend to have higher risks at a younger age, but after menopause, women’s risk rises.
While you can’t control your age or genetics, adopting heart-healthy habits can significantly lower your overall risk.
3. Strategies to Prevent Atherosclerosis and Heart Disease
A combination of lifestyle changes, medical interventions, and routine health monitoring can help manage cholesterol levels and reduce cardiovascular risk.
A. Maintain a Heart-Healthy Diet
- Increase fiber intake – Foods rich in soluble fiber (oats, beans, flaxseeds) help lower LDL cholesterol.
- Choose healthy fats – Focus on unsaturated fats from olive oil, nuts, and avocados.
- Limit saturated and trans fats – Found in red meat, fried foods, and processed snacks, these fats contribute to cholesterol buildup.
- Eat omega-3-rich foods – Fatty fish (salmon, mackerel, sardines) help lower triglycerides and inflammation.
- Reduce sugar and refined carbohydrates – Excess sugar contributes to weight gain, insulin resistance, and high cholesterol.
B. Exercise Regularly
Physical activity helps increase HDL cholesterol, lower LDL cholesterol, and maintain a healthy weight. Recommended activities include:
- Aerobic exercises (walking, jogging, cycling) – 150 minutes per week.
- Strength training (weightlifting, resistance exercises) – 2–3 times per week.
- Flexibility and balance exercises (yoga, stretching) – To support overall well-being.
C. Maintain a Healthy Weight
Excess weight, especially around the abdomen, increases cholesterol and heart disease risk. Losing even 5–10% of body weight can significantly improve cholesterol levels.
D. Quit Smoking and Limit Alcohol Intake
- Smoking cessation improves artery function and raises HDL levels.
- Limit alcohol consumption to moderate levels (1 drink per day for women, 2 for men), as excess alcohol can raise triglycerides.
E. Manage Stress Effectively
Chronic stress contributes to high blood pressure, inflammation, and unhealthy habits like overeating. Try:
- Meditation and deep breathing
- Yoga or tai chi
- Spending time in nature
- Healthy social connections
F. Monitor and Manage Medical Conditions
- Control high blood pressure through lifestyle changes or medication.
- Manage diabetes with diet, exercise, and proper medication.
- Regular cholesterol screenings help catch issues early.
4. When Medication Is Needed
For individuals at high risk of heart disease or those who cannot control cholesterol through lifestyle alone, medications may be necessary. These include:
- Statins – First-line treatment to lower LDL cholesterol.
- PCSK9 inhibitors – Used for severe cases or genetic high cholesterol.
- Ezetimibe – Blocks cholesterol absorption from food.
- Fibrates and niacin – Help lower triglycerides.
Medications work best when combined with healthy lifestyle changes.
5. The Importance of Regular Check-Ups
Even if you feel healthy, routine medical check-ups are essential for preventing complications. Your doctor may recommend:
- Lipid panel tests to monitor cholesterol levels.
- Blood pressure checks to prevent hypertension.
- Blood sugar tests to detect early diabetes.
- Electrocardiograms (ECG) or stress tests for heart function evaluation if at high risk.
Early intervention is key—catching and addressing cholesterol problems before they cause major heart issues can save lives.
Final Thoughts
Preventing heart disease starts with managing cholesterol and controlling risk factors. By adopting a heart-healthy lifestyle, regularly monitoring your health, and seeking medical treatment when necessary, you can significantly reduce your risk of complications like atherosclerosis, heart attacks, and strokes. Taking small steps today leads to a longer, healthier future with a strong heart.
Conclusion
Maintaining healthy cholesterol levels is essential for overall heart health and preventing serious conditions like atherosclerosis, heart attacks, and strokes. Understanding the difference between LDL (“bad”) cholesterol, HDL (“good”) cholesterol, and triglycerides can help you take proactive steps to manage your levels effectively.
While high cholesterol often shows no symptoms, routine testing is the key to early detection and prevention. A heart-healthy diet rich in fiber, omega-3 fatty acids, and healthy fats, combined with regular physical activity, weight management, and lifestyle modifications, can significantly improve your cholesterol profile. In some cases, supplements and medications may be necessary for better control, especially for those at higher risk.
By taking a proactive approach to your heart health—through healthy habits, regular check-ups, and, when needed, medical interventions—you can reduce your risk of cardiovascular disease and enjoy a longer, healthier life. Small changes today can lead to a big impact on your well-being in the future.